
Having your baby…the Northumbria way
This is such a special time in your life and we want you to have the best possible experience. We’re here to offer you lots of support throughout pregnancy, during birth and after the birth of your baby.
All pregnant women booked to deliver their baby with Northumbria Healthcare are offered their recommended pregnancy vaccinations at their routine ultrasound scan appointments. This includes seasonal flu (Sept – March), pertussis (whooping cough) and the Covid-19 booster when applicable. From 1 September 2024, all pregnant women will be offered the RSV (Respiratory Syncytial Virus) vaccination when they are 28 weeks pregnant.
For more information on recommended vaccinations in pregnancy:
RSV vaccination - A guide to RSV vaccination for pregnant women - GOV.UK (www.gov.uk)
Seasonal flu - https://
Pertussis (whooping cough) - https://
RSV vaccination
What is it?
From 1 September 2024, pregnant women can have a free vaccine in each pregnancy, to protect their babies against respiratory syncytial virus (RSV). The vaccine is offered from 28-weeks of pregnancy.
RSV is a common virus which can cause a lung infection called bronchiolitis. In small babies this condition can make it hard to breathe and to feed. Most cases can be managed at home but around 20,000 infants are admitted to hospital with bronchiolitis each year in England. Infants with severe bronchiolitis may need intensive care and the infection can be fatal. RSV is more likely to be serious in very young babies, those born prematurely, and those with conditions that affect their heart, breathing or immune system.
How will it protect my baby?
The vaccine boosts your immune system to produce more antibodies against the virus. These antibodies then pass through the placenta to help protect your baby from the day they are born. RSV vaccination reduces the risk of severe bronchiolitis by 70% in the first 6 months of life. After this age your baby is at much lower risk of severe RSV.
Is it safe?
The vaccine has been studied in clinical trials of almost 4,000 women and been given to many thousands of women in national programmes.
Monitoring in the USA, where it has been given to over 300,000 women, has shown a good safety profile. The vaccine has been approved by medicines regulators in the UK, Europe and USA on the basis of protection, quality and safety. For more information: Why vaccination is important and the safest way to protect yourself - NHS
Pregnancy vaccination sessions
Vaccines are available in the Antenatal Clinics at North Tyneside and Wansbeck Hospitals, Monday - Friday 09:00 - 16:00. You will be offered your vaccinations during your routine clinic antenatal clinic appointment. If you are unable to attend, or miss an appointment, we have drop-in sessions available every Friday at North Tyneside and Wansbeck Antenatal Clinics.
If you see your Midwife in one of our Midwifery Led Units, you will be offered your vaccination there. Please speak to your midwife for more information.
For more information on vaccination appointments, please call our dedicated vaccination team on: 0191 3499643.
You can also drop in to North Tyneside General Hospital Antenatal Clinics every Friday 9:00 am - 4:00 pm for your vaccines - no appointment needed.
New 'Drop In' clinics available
We will be offering a postnatal contraception service at our weekend postnatal clinics from 21st June 2025. .
We can offer:
- Progesterone-only pill (mini pill)
- Contraceptive injection
- Contraceptive implant
All contraception offered by maternity is safe to use immediately after birth and when breastfeeding.
Just drop in, babies and other children are welcome to attend. No appointment necessary.
Clinics will run on alternate weekends on the following dates:
21st June: NTGH Antenatal Clinic (maternity entrance)
28th June: WGH Antenatal Clinic (next to main outpatients)
5th July: NTGH Antenatal Clinic (maternity entrance)
12th July: WGH Antenatal Clinic (next to main outpatients)
19th July: NTGH Antenatal Clinic (maternity entrance)
26th July: WGH Antenatal Clinic (next to main outpatients)
Clinics will run weekly at both sites after this initial period.
For more information on postnatal contraception: Sex and contraception after birth - NHS
Found out you're pregnant?
Have you found out you're pregnant? Watch the short video below for guidance and to know about the next steps you need to take:
Self-referral to Northumbria Maternity
From December 5 2022, any pregnant person in the North Tyneside or Northumberland area will be able to directly refer themselves into the maternity service at Northumbria Healthcare NHS Foundation Trust. This short video from our Digital Midwife, Gayle Thompson, gives you more information about these changes.
How to refer yourself into Northumbria Maternity
As soon as you find out you are pregnant you are able to book for maternity care directly with Northumbria Healthcare Maternity Services instead of contacting your GP. We recommend that you do this as soon as possible so that we can arrange your 1st booking appointment for between 8 – 10 weeks. This also helps us offer screening tests for you and your baby at the correct stage in your pregnancy.
Once you have confirmed your pregnancy and you are more than six weeks pregnant, please follow the simple steps below to register with the service:
STEP 1 - Get your NHS number
Ensure you have your NHS number before filling in the form. If you don’t know yours, click here to get it
STEP 2 - Check you dates
It is important to know the first date of your last menstrual period to ensure you have your booking appointment in time for important screening tests. If you are unsure, please provide a date as close to that as possible.
STEP 3 - Complete this registration form
What happens next?
Once you have submitted the registration form, a member of our community midwifery team will contact you by telephone to arrange your booking appointment. They will also give you access to your electronic hand-held records called Badgernotes.
Women who do not have internet access will be able to contact the service by phone to register for their pregnancy care.
Screening tests are used to find people at higher chance of a health condition. Whether or not to have each test is a personal choice that only the individual invited for screening can make.
We offer all pregnant women screening tests during pregnancy to look for certain health conditions that could affect them or their baby.
Screening tests are also offered for babies soon after they are born so they can be given appropriate treatment as quickly as possible if needed.
Read the screening tests for you and your baby leaflet before your midwife booking appointment to find out much more about the screening tests offered during and after pregnancy. This information is also available in other languages and easy guides.
If you need one, you can pick up a printed copy of this leaflet at your booking appointment.
Antenatal screening programmes:
- Sickle cell and thalassaemia
- Infectious diseases
- Down’s/Edward’s/Patau’s syndrome and fetal anomaly ultra sound scan
Newborn screening programmes:
- Hearing screening
- Blood spot screening
- Newborn and infant physical examination
The screening programmes will be discussed with you at the appropriate time, either during your pregnancy or after the birth of your baby. You will have time at your appointments to discuss your options and have any queries that you may have answered.
More information about these programmes are available in your ‘screening tests for you and your baby’ leaflet given to you at your early pregnancy session/booking appointment. You can find more information on screening on NHS Choices here.
Birth centre
If you’ve chosen to have your baby with us at the Northumbria hospital, watch our video to familiarise yourself with our department and what will happen upon your arrival.
Midwife Led Units (MLUs)
Our three MLUs are open seven days a week, from 8.30am to 6pm on week days and from 9am to 2.30pm on weekends and bank holidays, with antenatal clinics, consultant-led clinics, postnatal drop-in clinics and community midwifery services.
The units have an overnight on-call system for women deemed to be low-risk who are due to give birth at the MLU’s and at home. Find out more here.
Berwick Infirmary:
Hexham General Hospital:
Alnwick Infirmary:
Home birth
If you have a straightforward pregnancy, and both you and the baby are well, you might choose to give birth at home.
For more information on where to give birth please visit: Where to give birth: the options - NHS (www.nhs.uk)
Midwife Led Care
During pregnancy most of your contact will be with your community midwife who will see you regularly to ensure that both you and your baby are healthy and to answer any questions you may have.
As soon as you have a positive pregnancy test your GP surgery will provide you with the information you need to access the care of one of our community midwives. Please watch the video at the top of the page for more information on early pregnancy including screening tests.
Once you have received this information, you should feel able to make informed decisions about your care and where you would like to have your baby. A booking appointment is then planned to discuss these decisions and your care during your pregnancy and after you have your baby.
You will be offered two ultrasound scans at a hospital of your choice. The first scan, in early pregnancy, is to confirm the expected date of delivery and the second scan is to assess your baby’s development.
You will also be offered parent education classes and given an appointment to attend an infant feeding workshop.
Throughout your pregnancy, information and advice is available to you from all the health professionals involved in your care. We have many leaflets readily available which may help you understand, and make decisions on, your care and treatment. The information most appropriate to you will be provided to you throughout your care and you can talk to your midwife or health professional at any point for more advice.
Low risk pregnancies do not generally require a consultant appointment, the midwife is responsible for your care. Your health, and your baby’s development will be reviewed at each appointment during your pregnancy. Additional appointments or a change to your pathway of care may be recommended if there are any concerns.
Consultant Led Care
Should you require any extra care (or you are deemed high risk) your midwife will refer you to the hospital to see a consultant or specialist midwife.
Antenatal clinics are held in a variety of settings, including GP surgeries, children’s centres and in our hospitals to give you a choice of time and location that is most convenient for you. Your community midwife will provide you with the information you need to decide where to have your antenatal care, including those clinics run by our specialist midwives.
Northumbria Maternity is now using BadgerNet and BadgerNotes, a fully digital pregnancy care record which allows you real time access to your maternity record. BadgerNotes can be downloaded from the App Store. You will receive log in details and a password when you attend your booking appointment with your Midwife. For more information visit https://

Women with a multiple pregnancy are cared for by a core multidisciplinary team. All women with multiple pregnancies require increased monitoring and will receive additional appointments and scans.
Some women already have high blood pressure (hypertension) before they become pregnant and they may be on treatment for this. You can also develop high blood pressure whilst you are pregnant, which returns to normal after your baby is born. This is called gestational hypertension.
There is a separate, less common condition called pre-eclampsia which can develop during pregnancy. This involves high blood pressure as well as other symptoms. This condition can become serious and needs extra care.
If you have any problems with your blood pressure, either before pregnancy or which develop during pregnancy, you will receive additional monitoring and appointments with the multidisciplinary team.
We also have the option of home blood pressure monitoring, which will be discussed with you at your appointments.
Women who have a history of one previous delivery by lower segment caesarean section (LSCS) may wish to consider a vaginal delivery in their subsequent pregnancy. The chance of successful vaginal delivery is between 72-75% (RCOG, 2015).
If you have given birth by LSCS previously, you will receive be offered additional consultant appointments, where midwives and obstetric staff will provide you will provide you with support and evidence-based information to enable you to make an informed choice regarding VBAC.
See leaflet here for more information
We run a monthly ‘Next Birth After Caesarean Section’ antenatal session via Zoom. The session is hosted by experienced clinicians who can answer all of your questions and provide you with the most up to date evidence to support your decision.
Book your place via Eventbrite here
.
Pre-existing diabetes
Patients with pre-existing diabetes will receive care from a team of specialist midwives and consultants. An individual management plan will be developed with the patient and the specialist team, including antenatal care, labour care and a postnatal care plan.
Most pregnant women with diabetes will go on to have a healthy baby, but there are some possible complications you should be aware of.
If you have type 1 or type 2 diabetes, you may be at higher risk of having:
- a large baby – which increases the risk of a difficult birth, having your labour induced or needing a caesarean section
- a miscarriage
People with diabetes are at risk of developing problems with their eyes (diabetic retinopathy) and kidneys (diabetic nephropathy).
Some people with type 1 diabetes can develop diabetic ketoacidosis, where harmful chemicals called ketones build up in the blood.
Pregnancy can increase your risk of developing these problems or make existing ones worse.
The best way to reduce the risks to you and your baby is to ensure your diabetes is well controlled before you become pregnant. Before you start trying for a baby, ask your GP or diabetes specialist for advice. You should be referred to a diabetic pre-conception clinic for support.
Gestational diabetes (GDM)
Gestational diabetes is high blood sugar (glucose) that develops during pregnancy and usually disappears after giving birth. It can happen at any stage of pregnancy, but is more common in the second or third trimester.
It happens when your body cannot produce enough insulin – a hormone that helps control blood sugar levels – to meet your extra needs in pregnancy.
Gestational diabetes can cause problems for you and your baby during pregnancy and after birth. But the risks can be reduced if the condition is detected early and well managed.
If you are diagnosed with GDM in your pregnancy, you will receive care from a team of specialist midwives and consultants. An individual management plan will be developed with you, including antenatal care, labour care and a postnatal care plan.
For more information, see Diabetes UK's information here.
At your booking appointment, you will be assessed for a variety of risk factors, including those that would make you at higher risk of preterm birth (less than 37 weeks gestation). If you are identified as being at risk, you will receive additional care from our specialist pre-term birth clinic.
An individual care plan will be developed with you in consultation with the specialist team.
Take a look at the short video below about premature labour questions answers by our public health midwife, Carla Anderson.
Your midwife will discuss your mental health history with you at the booking appointment and assess your wellbeing throughout your pregnancy.
If you have a history of mental ill health, you will be cared for by a consultant and specialist multi-disciplinary team.
We work with a number of services to support you depnding on your individual circumstances.
Your midwife will calculate your BMI at your booking appointment and advise you accordingly. Patients with a BMI over 35 receive care from a specialist team of midwives and consultants. You may also receive an assessment from an anaesthetist if your BMI is very high.
Having a high BMI when pregnant increases the risk of pregnancy and birth complications and can have an effect on your unborn baby.
There are lots of services which can help you be physically active and eat well during your pregnancy and develop healthier habits for life. Your midwife can refer you to these services at your booking appointment or any stage in pregnancy.
If you live in Northumberland, your midwife will refer you to a ‘Health Trainer’ who will work with you to develop a personalised well being plan to promote a healthy pregnancy. Health Trainers are specially trained to support you to achieve your personal goals and to have a healthier pregnancy.
If you live in North Tyneside, your midwife will refer you to a Health Coach, who are trained to support you to make healthier choices to improve your wellbeing. The Health Coach can refer you on to other services such as Active North Tyneside specialist classes and support.
We work closely with our colleagues in Physiotherapy and Health Psychology to support women with a high BMI, a referral into these services may be discussed with you.
More information about having a healthier pregnancy here.
Smoking during pregnancy has huge risks for the health and development of your baby. Quitting smoking during pregnancy is the single most important thing you can do to protect your baby’s health.
All women receive carbon monoxide monitoring as routine practice at every antenatal appointment. If you are identified as a smoker, you will be referred onto a high-risk pathway of care where you will be cared for by a specialist midwife and reviewed by a consultant.
We can help you to quit smoking at any point in pregnancy, but the earlier you try, the lower the risk of complications to your baby. Your midwife will refer you to specialist stop smoking services who will support you to quit.
More information on help available can be found here.
Incentive scheme
We offer Love2Shop vouchers as an incentive to remain smokefree during pregnancy.
Vouchers are offered to all women who set a quit attempt and who remain quit throughout pregnancy, this is monitored by regular carbon monoxide testing.
For more information, speak to your midwife or Best Start in Life Advisor
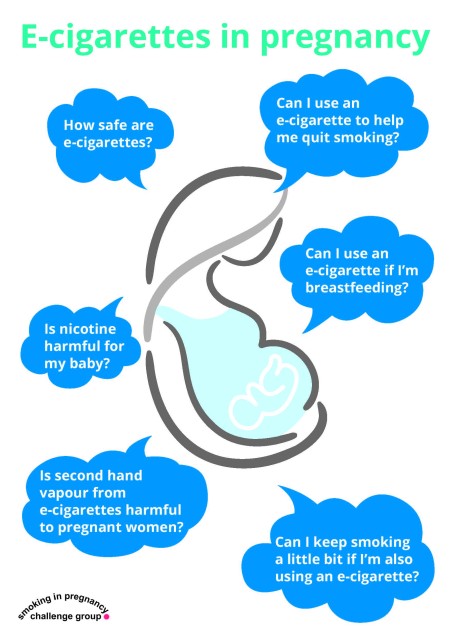
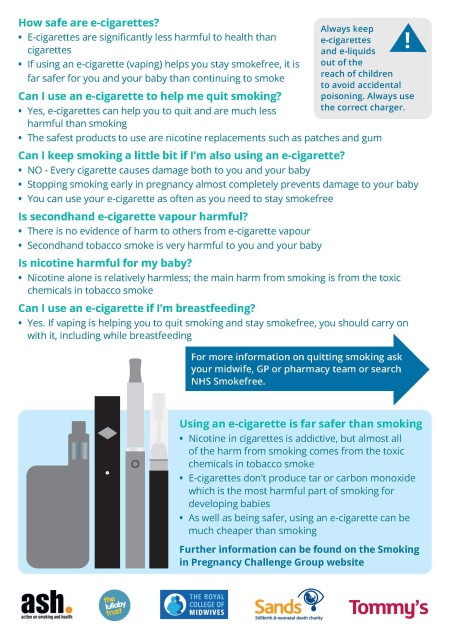
E-Cigarettes in pregnancy
Is it safe to drink alcohol when pregnant?
The Chief Medical Officers for the UK recommend that if you’re pregnant or planning to become pregnant, the safest approach is not to drink alcohol at all to keep risks to your baby to a minimum.
Drinking in pregnancy can lead to long-term harm to the baby, with the more you drink, the greater the risk.
Illegal drugs in pregnancy
Using illegal or street drugs during pregnancy, including cannabis, ecstasy, cocaine and heroin, can have a potentially serious effect on your unborn baby.
If you regularly use drugs, it’s important to tackle this now you’re pregnant.
It’s best not to stop abruptly without first seeking medical advice as there may be withdrawal problems or other side effects.
Getting help
If you use drugs or need help to stop drinking alcohol, it’s important to seek help straight away so you can get the right advice and support. Speak to your midwife who will ensure you receive the help you need with no judgement, just support.
For more information visit our alcohol and substance misuse during pregnancy page.
Useful links
Maintaining a healthy weight and continuing to exercise is very important during pregnancy and after birth. We can support you to stay healthy throughout pregnancy. Our Health Coaches and Health Trainers will work with you to provide an individualised plan for your wellbeing. Speak to your midwife for more information and to be referred.
Even small amounts of movement can make a really big difference to you and your baby’s health. Our physiotherapy team have recorded this video which is really helpful for anyone new to exercise or who wants to try some gentle activity:
There are some great tips, advice and videos on how to stay active on This Mum Moves. This is also available via the Baby Buddy App.
For foods to avoid and healthy eating advice during pregnancy, click here
Rise have worked with Northumbria NHS Foundation Trust to create this video to support women to walk whilst pregnant. Walking is a great form of activity to undertake when pregnant for almost all women because:
- It is safe for you and baby
- It can improve birth outcomes
- It is free
- You can fit it easily into your life both before and after birth
- It is a great social opportunity or a chance to catch up with friends
- It can support mental health and wellbeing
Please speak to your midwife if you have any concerns or for further advice around exercise during pregnancy
The Active Pregnancy Foundation website has a activity-based resources packed with advice and top tips to support you on your active journey through pregnancy and beyond. Click here to visit the website.
Our Parentcraft team have developed a programme of virtual antenatal education classes which you are welcome to attend via Zoom.
Book your place via Eventbrite here

What is induction of labour?
Most pregnancies will end between 37 and 42 weeks when labour starts naturally and results in the birth of the baby. Induction of labour is a process that starts your labour artificially. On average one in five women may have their labour induced and your individual circumstances can be discussed with your midwife or consultant.
Hear from our advanced clinical practitioner, Julie Wyton about the induction of labour process.
When might induction be recommended?
Induction of labour is usually offered at 41 weeks of pregnancy if labour has not started naturally. The choice to proceed with Induction of Labour is yours once you have received all of the relevant information. You may find the NHS Choices leaflet helpful when making your decision
Induction of labour will be recommended if there are concerns that you or your baby’s health would be at risk if your pregnancy continued.
Some examples of medical reasons for induction include:
- High blood pressure
- Diabetes
- Small baby
If your waters break early you will be offered induction of labour at 37 weeks. A doctor will discuss this with you.
You can find more information here.
Monitoring your baby’s heartbeat during labour:
We want you to have a healthy baby and the best possible experience of birth. In order to achieve this, there are some checks we will do to make sure that you are both coping well. For mum, this will include checking your temperature, pulse and blood pressure regularly.
For baby, we can monitor your baby’s heartbeat. This is called fetal heart monitoring and is the same as checking your bay’s pulse. Performing fetal heart monitoring allows us to assess your baby’s wellbeing.
Please see this leaflet for more information on types of fetal monitoring and the reasons for this.
There are many types of analgesia which you might like to try:
Self-help in labour
You’re likely to feel more relaxed in labour and better placed to cope with the pain if you:
- learn about labour – this can make you feel more in control and less frightened about what’s going to happen; talk to your midwife, ask them questions, and book on to our antenatal classes
- learn how to relax, stay calm and breathe deeply
- keep moving – your position can make a difference, so try kneeling, walking around, or rocking backwards and forwards
- bring a partner, friend or relative to support you during labour, but do not worry if you do not have a partner – your midwife will give you all the support you need
- ask your partner to massage you – although you may find you do not want to be touched
- have a bath
Water / birthing pool
Water is useful for managing pain in labour. It encourages you to relax and is thought to make the contractions seem less painful. The use of water for pain relief is available as long as there are no contraindications (factors that mean a birthing pool should not be used). The water will be kept at a temperature that is comfortable for you but not above 37°C. Your temperature will also be monitored closely. If any problems are detected with either you or your baby, you will be asked to leave the pool.
Hypnobirthing
We fully support birthing parents who wish to use hypnobirthing through their labour. You are welcome to discuss this with your midwife and add this to your birth plan so that all staff are aware of your choices.
- Hypnobirthing can help you manage stress hormones, such as adrenalin, and reduce anxiety, which should lead to a calmer birth. During labour, your body produces a chemical called oxytocin, which helps progress your labour. Stress hormones affect the production of oxytocin, and make your labour longer.
- Managing stress may also help to reduce some of the fear and pain experienced during labour.
- In some cases, hypnobirthing has been shown to make labour shorter.
- Practising hypnobirthing – whether it’s at a class, with a book or CD – may help you to feel more prepared and in control when labour starts.
- It may help you cope with anxieties if you had a previous traumatic birth experience.
- Hypnobirthing may reduce the need for drugs and medical intervention. However, you can have additional pain relief as well if you want to.
- It can be added to any birth plan and the techniques can be used wherever you give birth – in a hospital or birth centre, or at home.
- Hypnobirthing may benefit you after birth too, with some evidence showing that it can lower the chance of postnatal depression.
- Hypnobirthing can help your birth partner play a more active role during labour.
Tens machine
This stands for transcutaneous electrical nerve stimulation. We have a number of TENS machine available for you to use in all of our hospitals. TENS is believed to work by stimulating the body to produce more of its own natural painkillers, called endorphins. It also reduces the number of pain signals sent to the brain by the spinal cord.
TENS has not been shown to be effective during the active phase of labour, when contractions get longer, stronger and more frequent. It’s most effective during the early stages, when many women experience lower back pain.
Gas and air/Entonox
This is a mixture of oxygen and nitrous oxide gas. Gas and air will not remove all the pain, but it can help reduce it and make it more bearable. Many women like it because it’s easy to use and they control it themselves.
- You breathe in the gas and air through a mask or mouthpiece, which you hold yourself.
- The gas takes about 15-20 seconds to work, so you breathe it in just as a contraction begins.
- It works best if you take slow, deep breaths.
This is an injection of an opiate medicine into your thigh or buttock to relieve pain. It can also help you to relax. It takes about 20 minutes to work after the injection. The effects last between 2 and 4 hours.
Diamorphine/Pethidine injections (opioids)
There are some side effects to be aware of:
- it can make some women feel woozy, sick and forgetful
- if pethidine or diamorphine are given too close to the time of delivery, they may affect the baby’s breathing – if this happens, another medicine to reverse the effect will be given these medicines can interfere with the baby’s first feed
Epidural
An epidural is a type of local anaesthetic and is given by an anaesthetist. It numbs the nerves that carry the pain impulses from the birth canal to the brain. For most women, an epidural gives complete pain relief. It can be helpful for women who are having a long or particularly painful labour.
There is a pain relief comparison card here.
Whilst most birthing people choose to aim for a spontaneous vaginal delivery, there are alternative options for your delivery.
What is a caesarean section?
This is when your baby is delivered through a cut (incision) made in the lower part of your abdomen. Usually the incision is just below the pubic hair line (bikini line).
Caesarean sections are only performed at the Northumbria Specialist Emergency Care Hospital.
Elective Caesarean Section
A caesarean section is performed when it is thought that a vaginal delivery may cause concern for either the mother or baby. This can be for a number of reasons:
- If there are concerns about your baby’s wellbeing in the womb
- The pelvis is not big enough to allow the baby to pass through
- When the placenta is covering the neck of the womb (cervix)
- Sometimes if the baby is in the breech position (bottom first)
- If the neck of the womb (cervix) does not open up enough during induction or in labour
There are many other reasons why it might be necessary to perform a caesarean section. If you are not sure why you might need to have one then please ask your midwife or doctor to explain.
If you request a caesarean section the consultant obstetrician will discuss this with you.
Find out more about elective caesarean section Considering a caesarean birth patient information leaflet | RCOG
Emergency Caesarean section
The most common reason for this is immediate concern for the wellbeing of the baby. If the baby is showing signs of distress or is not coping and birth is not imminent, then an emergency caesarean section may be recommended.
Another reason for an emergency section may be if your labour has slowed or stopped and interventions to encourage progress have been unsuccessful. A very prolonged labour may be unsafe for you or your baby as it can lead to your baby becoming distressed and an increased chance you may bleed more heavily after birth.
Your midwife will stay with you and continue to care for you in theatre and after your baby is born.
Caring for your wound after a caesarean birth
Please see this leaflet for more information about caring for your wound after a caesarean birth.
Instrumental Birth
An instrumental delivery is where either suction cup or forceps are used to gently pull the baby down the birth canal, whilst the mother pushes to achieve a vaginal birth.
If it is recommended that you need an instrumental delivery, the reason for it will be clearly explained to you by the obstetrician. You will have the chance to ask questions and discuss your options so you can give your informed consent to the procedure. Your midwife will stay with you and continue to support you throughout the birth.
For more information about planning your pregnancy care, place of birth and what options are available for you in the region, the ‘Pregnancy and Birth Choices in the North East and North Cumbria Web App’ is a great resource.
We provide postnatal care for you and your baby up to 28 days post birth. Postnatal inpatient care is offered on Ward 16 at The Northumbria Hospital (NSECH), all rooms are private with en-suite facilities.
Birth partners are welcome to stay overnight, all other visitors must book a visiting time slot with the ward clerk. Postnatal care is continued by our team of community midwives who will visit you in your home or offer you an appointment in our postnatal clinic. If you have any concerns about your or your baby during the postnatal period, you should contact
We explain the fourth trimester
Signs and symptoms of an unwell baby
Signs and symptoms of an unwell mum
Choosing how you feed your baby is a personal choice and one that doesn’t need to be made before your baby is born. Although getting all the information when your pregnant will help you to make your decision. Your midwife and health visitor will be able to give you lots of information and answer any questions you may have.
Regardless of your feeding choice getting to know your baby during pregnancy helps your baby’s brain development. Take some time to relax and talk to your baby, stroke your bump. Encouraging your partner and other children to do the same will also help with the family bonding. Responding to your baby has been shown to be the most effective way of feeding, regardless of feeding choice so getting to know your baby early is a great way to start your feeding journey.
Skin to skin
Holding your baby in skin to skin directly after birth for at least an hour or until after the first feed, regardless of your feeding choice, will have benefits for both you and your baby. Skin to skin contact:
- Regulates your baby’s temperature, heart rate and breathing
- Calms and relaxes both you and your baby (and also your partner)
- Passes all the family friendly bacteria from mum to baby to help protect against infection
- Stimulates digestion ready for the first feed
For more information on skin to skin and the benefits and safety considerations, click here
Breastfeeding
Here at Northumbria we support all women to choose how they want to feed their baby, our staff are also aware of all the benefits that breastfeeding your baby brings to both you and your baby. Getting your feeding journey off to the best start will benefit both you and your baby health wise and also support the growing bond between you both. Our staff will be able to support you, antenatally and after your baby is born. Please speak to your midwife if you have any questions you would like answering.
Antenatal colostrum harvesting is a great way to commence your breastfeeding journey. By expressing your colostrum towards the end of your pregnancy you will be better prepared to meet any feeding challenges should they arise. For more information click here
Formula Feeding
It is important that formula feeds are sterilised and made up safely at the right time. Powdered infant formula is not sterile and needs to be made up at the right temperature which will kill any potential bacteria present.
Please see – Guide To Bottle Feeding for more information.
Making sure you get the right milk for your baby is really important, your baby can stay on the Stage 1 (often described as suitable for newborns) until they are one year old. For more information on formula milks and different brands, please go to: First Steps Nutrition
The early days with your baby are a great time to get to know and build that loving bond together. Keeping your baby close and responding to the feeding cues will ensure your baby is relaxed and feels secure. More information on responsive bottle feeding can be found here.
Tounge Tie
What is a tongue tie?
A tongue tie is an extra piece of skin which goes from underneath the tongue to the floor of the mouth and restricts the tongue’s movement.
Babies feed well with a free moving tongue regardless if they are breast or bottle fed. The presence of a tongue-tie may lead to feeding difficulties.
If a tongue tie is suspected to be causing your baby feeding difficulties, your midwife or health visitor will discuss with you a referral for a tongue tie assessment.
We have a specialist tongue tie division service at Northumbria for babies up to 6 weeks of age.
For lots more information on tongue tie, see our leaflet.
We have a team of Obstetric Physiotherapists who work across our Trust to keep you healthy and comfortable during your pregnancy and post-delivery. Below are some downloadable resources that you can access to guide you.
You can have both telephone or face to face consultations with a physiotherapist, so please ask your midwife to refer you.
We also have Fit for pregnancy classes running face to face at both Wansbeck General Hospital and North Tyneside General hospital. These classes are a great way to learn how your body changes during pregnancy (as these changes can contribute to aches and pains that you may experience), what it means to be physically active during pregnancy and ways to reduce discomfort.
Pregnancy resources
Pelvic Floor
What is my pelvic floor? How do I do pelvic floor exercises? In this video, a Specialist Pelvic Health Physiotherapist explains how to get started on finding your pelvic floor muscles and why you should be exercising these muscles as part of your daily routine. Pelvic Health Physiotherapists help with pelvic floor dysfunction caused by pregnancy and childbirth, or other issues including incontinence and pelvic pain.
For more information please see this leaflet: The Pelvic Floor Muscles - a guide for women
Posture and position during pregnancy
For more information please see this leaflet: Fit for pregnancy
If you are experiencing back and/or pelvic girdle pain during your pregnancy, watch our videos here for advice.
We also have multiple episodes on physiotherapy as part of our Maternity @ Northumbria podcast. Listen here
Bladder and vaginal problems during and after pregnancy
For more information please see this leaflet: Pelvic organ prolapse
Constipation during and after pregnancy
For more information please see this leaflet: Improving your bowel function
Back/pelvic pain during pregnancy
For more information please the following leaflets:
Physical activity during pregnancy
If you are keen to remain/start being active during your pregnancy please see this resource: Active Pregnancy Foundation
We also have multiple episodes on physiotherapy as part of our Maternity @ Northumbria podcast. Listen here.
Benefits of physical activity during pregnancy to health and well-being
Preparing for labour
Perineal massage
Guided meditation with Lesley Beattie - Pelvic, Obstetric and Breast Health Physiotherapist
Breathing exercises demonstration with Lesley Beattie - Pelvic, Obstetric and Breast Health Physiotherapist
Guided meditation with Mel Corbo - - Pelvic, Obstetric and Breast Health Physiotherapist
Labour Positions with Mel Corbo - - Pelvic, Obstetric and Breast Health Physiotherapist
Post-birth resources
Bladder care
For more information please see the following leaflets:
Pain management and wound care
For more information please see the following leaflets:
Your core muscles after birth
For more information please see the following leaflets:
Return to exercise
For more information please see this leaflet: Fit for the future
It is also important to be physcially active post-birth.
Returning to running
Keen to get back to running post-birth? We have a video explaining how this is achieveable.
Self Assessment for DRA
A Diastasis of the Rectus Abdomins refers to thinning and widening of the linea alba (connective tissue in the middle of the abdominal wall between the rectus abdominis muscles) with associated laxity of the abdominal wall. It is often referred to as the “mummy tummy”. In this video, we explain how you can self-assess for a DRA
One of our many strengths as midwives on the Birthing Centre is the creating of precious memories for families to remember those precious moments with their babies. However, these memories wouldn’t be possible without the support from a number of charities.
Our maternity service at Northumbria follows the National Bereavement Care Pathway. The pathway ensures all families experiencing a pregnancy loss are provided with the same high standard of care.
The Willow Room is our dedicated bereavement room and is situated on the Birthing Centre at The Northumbria. The room provides a homely feel with soft furnishings and lighting to create a calm atmosphere for bereaved families to meet and spend time with their baby
A reflective diary in the Willow Room offers families the opportunity to reflect on their own experiences. These documented powerful moments create the message to others, “They are not alone.”
- Teardrop, a charity initially set up by a small group of midwives at Ashington hospital many years ago, is now run by bereaved families. Teardrop have funded numerous equipment and soft furnishings for the Willow Room.
- 4Louis provides the Willow Room with memory boxes, ensuring all precious memories are encapsulated in a beautiful box. The 4Louis clay and ink prints within the box provide a tangible memory for parents to take home. Baskets of all sizes are also provided by 4Louis to keep baby safe and keep dignity intact.
- Remember My Baby is a charity that can provide beautiful images for families of their babies. These images are created by a professional photographer who will attend the Willow Room and spend unlimited time to create those precious images.
- Little Things is a charity that provide clothes for the smaller gestation of babies. These bespoke items of clothing ensure baby is dressed in a dignified way for the families and all staff coming into contact with babies. 4Louis provide angel pocket to place those tiny babies in, keeping them comfortable and safe
Training for staff in the topic of bereavement within maternity is provided by two bereavement midwives experienced in the bereavement field. The charities 4Louis, Beyond Bea and SANDS also provide bereavement training within the topic area, ensuring staff have up to date information to meet the needs of bereaved families.
Funeral arrangement can be daunting for many families dealing with the loss of a baby. Two bereavement midwives with experience in funeral arrangements are available to families, to guide them through this sensitive process. They also act as a point of contact for families following their discharge home from the Birthing Centre as many families often feel alone at this point of their bereavement journey.
Our Obstetrics and Gynaecology Health Psychology team provide specialist support to bereaved parents, both after their loss and in any subsequent pregnancies. If you would like more information, speak to your midwife, or you can self-refer into the service by calling 01670 564 095. For more information, click here
Continuity of Carer in Northumbria
The continuity of carer programme is an approach in which mums-to-be and their families have a named lead midwife, who is supported by a small dedicated team of midwives, for the duration of the pregnancy, birth and after their little one is born.
This approach has been driven from a national level and it is envisaged that it will build a strong relationship of trust over time between the mum-to-be and their midwife.
Research has shown that when women receive this model of care they benefit from reduced incidence of early pregnancy loss, reduced incidence of premature delivery, less intervention during labour and delivery, and increased satisfaction with their care. It also means that you are 7 times more likely to know your Midwife who cares for you during your birth experience.
Since launching in January 2020, we have two teams under our maternity services that have benefitted from the new approach. Our aim is that most women will receive continuity of carer throughout pregnancy, birth and beyond by April 2023.
For more information on Continuity of Carer see here.
Sometimes following a birth it is helpful to talk through your experience. If you’ve had your baby with us, you can spend time talking to a midwife through our birth reflection service. This is available here
What is an MVP?
Maternity Voices Partnerships were set up after the Better Births report published in 2016. There are MVPs across the country and the Northumbria MVP covers all of Northumberland and North Tyneside. The MVP works with health professionals and families using maternity services to ensure that service provision is what families want and that people are listened to.
So what does an MVP actually DO?
The MVP works with NHS maternity departments to make sure that the services provided are what pregnant people and their families actually want. We help plan service provision, we help develop leaflets and communication and we provide feedback.
Some of the things we have worked on include updating the way pregnant people with diabetes are looked after, making sure that the voices from more vulnerable communities are heard and planning care during COVID (including supporting birth partners at ALL births and antenatal appointments). We are currently looking at how parents are supported to make a decision about being induced as feedback is that women and pregnant people often feel they didn’t have any choice or it wasn’t properly explained.
Is it just for pregnant women?
The MVP is for anyone involved in maternity care – so pregnant women and pregnant people and also their families. It is multidisciplinary so we also have representatives from midwifery, obstetrics, gynaecology, physiotherapy and SCBU (and more!). If you are pregnant or have had a baby recently, it would be great to have your support.
How can I find out more or get involved?
We currently have a Facebook page that is public and a closed group that is just for service users (so no professionals unless they are using maternity services). We are working on a website so will let you know once it is up and running.
A closed Facebook group for service users
About Rae – the Chair of the MVP
I am mum to four boys and have experienced four very different births: a planned home birth with transfer to hospital, a textbook home water birth, a very emergency caesarean section with a baby in NICU and then an induction. However, all four were positive and empowering because of the care I received and the way my decisions were supported.
As a Trust, we are committed to understanding the experience of patients accessing our maternity services. We do this in a number of different ways to make sure we learn what has worked well for you, and what we may need to do to improve our services. The following includes some of the ways that we may ask you for feedback.
- Realtime: We work with a patient experience team that visit our wards and ask you to describe your experience of care whilst in hospital
- Postal Survey: you might be contacted by Patient Perspective who collect feedback on our services. This usually happens two weeks after you are discharged from care.
- Text Message: As part of the National Friends & Family Test, you might receive a text message asking you to rate your experience of the Maternity service.
- NHS Choices & Care Opinion: You can leave a review at either site which we allow us to learn from your feedback. A member of our Patient Experience Team monitors these comments and will respond to posts.
- Patient Stories: We collect stories from patients to gain an in-depth understanding of care. We use these for learning and development purposes.
- Patient Experience e-mail: Patients can send good news stories, reflections and share other views with us at Patient.
Experience @northumbria-healthcare.nhs.uk
We are really keen to continuously learn and improve. Your experience is important to us as we are committed to getting healthcare right for our patients. If you would like to give feedback about one of our services, we would warmly welcome any views that you wish to share with us.
Our Professional Midwifery Advocates are a group of midwives who work within Northumbria Healthcare Trust who are here to support you with birth choices. They are experienced practicing midwives who have completed further training with the aim to support and facilitate the practices and development of midwives to ensure safety for women and their babies in addition to receiving a high standard of care.
PMAs aim to ensure women and families receive guidance and information about the right type of care, in the right care setting.
They are here to support women and families as well as to give sound professional advice.
They are also here if you have concerns about your care, you and/or your midwife may contact a PMA.
Women are able to talk to a PMA in confidence with any issues relating to practice care provision.
They can meet with you and your midwife and/or one of the consultants in order to help you achieve the birth you want by acting as a resource and to assist in discussing your birth choices. They will provide evidence-based information to help you achieve your goal and ensure all aspects of your planned care are explained thoroughly.
You can contact the PMA team via e-mail at PMA2
As a birth partner, there are lots of practical things you can do to support during labour, whatever kind of birth you and you partner are planning for.
This includes:
- keeping your partner company and helping to pass the time during the early stages
- holding her hand, wiping her face and giving sips of water
- massaging her back and shoulders, and helping her move about or change position
- comforting her as labour progresses and contractions get stronger
- reminding her how to use relaxation and breathing techniques – ask the Midwife to show you how if you are unsure
- supporting her decisions, such as pain relief choices, even if they’re different from what’s in the birth plan
- helping to explain to the midwife or doctor what she needs – and help them communicate with your partner – which can help you both feel more in control of the situation
- telling her what’s happening as your baby is being born if she wants you to
Useful link for further information:
Your Feelings
Just because your partner is the one carrying the baby, it does not mean their pregnancy has no impact on you. Whether the pregnancy has been planned for months or years, or is unexpected, you’ll probably feel a range of emotions.
A baby means new responsibilities that you may not feel ready for, whatever your age. You and the mum-to-be may have mixed feelings about the pregnancy. It’s normal for both of you to feel like this.
The first pregnancy will change your life and change can be frightening, even if it’s something you’ve been looking forward to.
A message from our Health Psychology team:
Everyone has different strategies for coping with difficulty. We believe that anyone can encounter emotional distress at any time in their life and that the issues related to fertility, conception, pregnancy and gynaecological difficulties can be especially hard. Our Obstetrics and Gynaecology Health Psychology Service offers psychological assessment and therapy for women and couples who are experiencing emotional difficulties arising in pregnancy or as a result of childbirth, or associated with a gynaecological condition. You can find more information by following this link.
Useful external links for more support:
If you need urgent help with your mental health, please call the NHS 24 hr phone line for urgent assistance: 0303 123 1146
COVID-19 support and guidance for partners
We know that this is a worrying time and it will definitely not be how you had planned your parenting journey. Whilst attending appointments is still restricted, there are other ways which you can bond with your growing baby and support your partner.
- Babies can hear within the womb from around 18 weeks. So, however silly it might feel, take time every day to speak, sing and read to your baby in the womb. This is the beginning of a life long bonding process which promotes brain development even before your baby is born
- Make sure that you get that crucial skin-to-skin contact as soon after birth as you can. Tell the midwife that you’d like to do this so it isn’t forgotten. Skin-to-skin is a great way for dads to continue to get close to their baby in the coming months.
- Skin-to-skin cuddles let your baby hear your heartbeat and learn your smell, just like they do with mum if she’s breastfeeding. Take every opportunity you can to let them snuggle up on your chest. It’s a lovely way to feel close and can help you both relax too. (NCT, 2020)
It is important that when the time comes, you bring a ‘hospital bag’ for yourself and please be aware that if your partner is having labour induced, you should be prepared for a stay of at least 3 days.
Useful items could include:
- Sandwiches and snacks (including pot noodles/pasta pots for which we can provide hot water)
- Treats for you and your partner – chocolate/sweets etc
- Books/puzzles to keep occupied prior to active labour
- iPad/tablet with downloaded films/series
- Toiletries for yourself
- Changes of clothing
Coping with Crying during lockdown
It is hard at the best of times coping with a crying baby. However, it is much more difficult when you are confined to the house and separated from your usual activities and support from family and friends. Follow this link for tips on coping with crying.
General tips for coping with a new baby, especially during COVID-19.
Smoking
A smoke free environment is recommended for you and your new family. Your partner’s midwife can refer you to the stop smoking service, which is a free service available to you. Ask your partner’s midwife to refer you, or your partner can ask on your behalf if you are not able to attend.
Alternatively you can visit here for further support to help you quit and give your baby a healthier start in life.
There is also a new Smoke Free App to support you to give up smoking.
Alcohol
It is advised that women don’t drink alcohol during pregnancy due to the affects this can have on the unborn baby, you can support your partner by also stopping or cutting down. There’s a strong link between heavy drinking and depression, hangovers can make you feel anxious and low. If you already feel anxious or sad, drinking can make this worse, so cutting down can make you feel in a better mood.
Drinking can also affect your sleep, it can help you fall to sleep quickly but with a new baby to care for during the night, drinking alcohol could make you less supportive and also poses a danger to your new baby.
For support with cutting down or stopping completely, click here
Whether you’ve just found out you are pregnant, or if you are halfway through your journey, our midwives have pulled together a series of videos to support you throughout your pregnancy. From exercise routines to methods of pain relief during labour, we’ve got you covered. Why not check them out here?
- Lateral flow testing for pregnant people and their support partners
- NHS Choices Pregnancy Care Planner
- National Childbirth Trust
- Man health
- Advice and guidance from the Northern Local Maternity System
- Hospital Bag Checklist
- Antenatal Colostrum Harvesting
- How to look after yourself at home if you have coronavirus (COVID-19)
- Pregnancy and coronavirus
- Group B Streptococcus information
- COVID19 vaccine information for pregnant people, breastfeeding and those planning a pregnancy
- If you have epilepsy and are pregnant
- Shared decision making tool
- Pregnancy assesment unit, Northumbria Specialist Emergency Care Hospital 0191 607 2815
- Birthing unit, Northumbria Specialist Emergency Care Hospital 0191 607 2318
- Hillcrest midwife-led unit 01665 626 732
- Berwick midwife-led unit 01289 356 622
- Hexham midwife-led unit 01434 655 352
Patient support groups
- Tamba (Twins) 01483 304442
- National Breast Feeding Helpline 0300 100 0212
- Newcastle Women’s Aid 0191 275 2148
- North Tyneside Woman’s Aid 0191 251 3305 / Out of hours 07946 753638
- Sexual Health Services 0344 728 0554
- Parentline Plus 24 hour parent advice line 0808 800222
Healthy Start
What is Healthy Start?
If you’re more than 10 weeks pregnant or have a child under 4, you may be entitled to get help to buy healthy food and milk. You can also receive free vitamins for you and your baby.
If you’re eligible, you’ll be sent a Healthy Start card with money on it that you can use in lots of UK shops.
Find out more and if you are eligible: Get help to buy food and milk (Healthy Start)
Eating well
Eat Well, Spend Less Eat-well-Spend-less-food-fact-sheet.pdf (bda.uk.com)
General information on a healthy diet in pregnancy Have a healthy diet in pregnancy - NHS (www.nhs.uk)
Finance/bills
Citizens advice Get help with the cost of living - Citizens Advice
Cost of heating homes
For information on help with energy bills see here.
Local support services
If you live in Northumberland, Northumberland Frontline is a one-stop shop webpage with all available services in Northumberland: https:/
If you live in North Tyneside, information on local services is available here: https://
Safe Sleeping
Keeping infants warm in colder homes may be raising concerns. This must be balanced with the risk of unsafe sleeping arrangements which include over wrapping.
The Lullaby Trust has new guidance on keeping babies warm and safe this winter see here. This includes messages on what is not recommended .
The following resources have been produced by the NENC Learning Disability Network to improve access to information for women:
A guide to Pregnancy - Easy Read
How will my baby be born? - Easy Read
What is a Forceps birth - Easy Read
What is a Ventouse birth? - Easy Read
Caesarean Section Information - Easy Read
Caesarean Section Consent Form - Easy Read
Contraception after having a baby - Easy Read
Contraception: The Implant - Easy Read
Contraception: Condoms - Easy Read
Female Urinary Catheter - Easy Read
Streroids in late pregnancy - Easy Read
Screening tests for you and your baby: Easy Guides
Maternity research is important as it helps improve experiences and outcomes for women and babies.
We regularly participate in research studies that have been approved by the National Institute for Hwalth Research (NIHR). You may be contacted by the maternity research team to ask if you would like to participate in a research study. You will always have the opportunity to discuss any study with your healthcare team and are under no obligation to participate.
See below the stuides that are currently being delivered within Northumbria Maternity:
INGR1D2
Investigating Genetic Risk for type 1 Diabetes (2) - is an important study that aims to identify children with genetic markers that put them at increased risk of developing type 1 diabetes. Find out more about this study The INGR1D 2 study
MiNESS 20-28
This study will look at medical factors associated with healthy birth and those associated with early stillbirth but also environmental, lifestyle and healthcare factors that can affect pregnancy and the wellbeing of the baby. Find our more about this study Research & Innovation
iGBS3
Northumbria maternity is participating in a research study of women’s natural immunity against GBS. We want to find out how much antibody a woman needs in her blood to protect her baby from getting GBS. This will help in developing a vaccine. Find out more about this study.
OBSUK Study
This research is part of a study called OBS UK aiming to improve care for women who bleed during childbirth. Find out more about this study.
Video consultations

We can offer online consultations where appropriate via a video call to make it easier for you to attend.
Rather than travelling to your appointment, you will receive a text or email before your appointment and simply need to click to join. Find out more here.



